Topic Overview
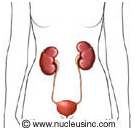 What are kidney stones? What are kidney stones?
Kidney stones are made of salts and minerals in the urine that stick together to form small "pebbles." They can be as small as grains of sand or as large as golf balls. They may stay in your kidneys or travel out of your body through the urinary tract. The urinary tract is the system that makes urine and carries it out of your body. It is made up of the kidneys, the tubes that connect the kidneys to the bladder (the ureters), the bladder, and the tube that leads from the bladder out of the body (the urethra).
When a stone travels through a ureter, it may cause no pain. Or it may cause great pain and other symptoms.
Cause
Kidney stones may form when the normal balance of water, salts, minerals, and other substances found in urine changes. How this balance changes determines the type of kidney stone you have. Most kidney stones are calcium-type—they form when the calcium levels in your urine change.
Factors that change your urine balance include:
- Not drinking enough water. Try to drink enough water to keep your urine clear (about 8 to 10 glasses of water a day). When you don't drink enough water, the salts, minerals, and other substances in the urine can stick together and form a stone. This is the most common cause of kidney stones.
- Medical conditions. Many medical conditions can affect the normal balance and cause stones to form. Gout is one example. Also, people who have inflammatory bowel disease or who have had surgery on their intestines may not absorb fat from their intestines in a normal way. This changes the way the intestines process calcium and other minerals, and it may lead to kidney stones.
More commonly, kidney stones can run in families, as stones often occur in family members over several generations.
In rare cases, a person forms kidney stones because the parathyroid glands produce too much of a hormone, which leads to higher calcium levels and possibly calcium kidney stones.
Symptoms
Kidney stones form in the kidney. If they stay in the kidney, they do not typically cause pain. When they travel out of the body through the tubes of the urinary tract (including the ureters, which connect the kidney to the bladder, or the urethra, which leads outside the body), their movement may cause:
- No symptoms, if the stone is small enough.
- Sudden, severe pain that gets worse in waves. Stones may cause intense pain in the back, side, abdomen, groin, or genitals. People who have had a kidney stone often describe the pain as "the worst pain I've ever had."
- Feeling sick to the stomach (nausea) and vomiting.
- Blood in the urine (hematuria), which can occur either with stones that stay in the kidney or with those that travel through the ureters.
- Frequent and painful urination, which may occur when the stone is in the ureter or after the stone has left the bladder and is in the urethra. Painful urination may occur when a urinary tract infection is also present.
Conditions with similar symptoms include appendicitis, hernias, ectopic pregnancy, and prostatitis.
What Happens
A kidney stone begins as a tiny piece of crystal in the kidney. When the urine leaves the kidney, it may carry the crystal out, or the crystal may stay in the kidney. If the crystal stays in the kidney, over time more small crystals join it and form a larger kidney stone.
Most stones leave the kidney and travel through the urinary tract when they are still small enough to pass easily out of the body. No treatment is necessary for these stones. But larger stones may become stuck in the tubes that carry urine from the kidney to the bladder (ureters). This can cause pain and possibly block the urine from flowing to the bladder and out of the body. The pain often becomes worse over 15 to 60 minutes until it is severe. The pain may ease when the stone no longer blocks the flow of urine, and it often goes away when the stone passes into the bladder. Medical treatment is often necessary for larger stones.
- The smaller a stone is, the more likely it is to exit the body (pass) on its own. About 9 out of every 10 stones smaller than 5 mm (0.2 in.) and about 5 out of every 10 stones 5 mm (0.2 in.) to 10 mm (0.4 in.) pass on their own. Only 1 or 2 out of every 10 kidney stones need more than home treatment.1
- The average time a stone takes to pass ranges between 1 and 3 weeks, and two-thirds of stones that pass on their own pass within 4 weeks of when the symptoms appeared.
- Almost half of all people who get kidney stones will get more stones within 5 years unless they take preventive measures. When you have kidney stones several times over a period of years, the length of time between stones tends to get shorter. It is not possible to predict who will have more stones in the future and who will not.
Problems that may occur with kidney stones include:
- An increased risk of urinary tract infection, or making an existing urinary tract infection worse.
- Kidney damage, if stones block the flow of urine out of both kidneys (or out of one kidney, for people who have a single kidney). For most people with healthy kidneys, kidney stones do not cause serious damage until they completely block the urinary tract for 2 weeks or longer.
Kidney stones are more serious for people who have a single kidney or an impaired immune system or have had a kidney transplant.
Stones in pregnant women
When stones occur during pregnancy, an obstetrician and urologist should determine whether you need treatment. Treatment will depend on your trimester of pregnancy.
Stones in children
Kidney stones are not common in children. When they occur, it is usually between the ages of 8 and 10. Children with kidney stones may also have a urinary tract infection. Children who have stones often have other medical problems, such as an abnormally developed urinary system, a metabolic disorder, or genetic risks, such as cystic fibrosis.
What Increases Your Risk
Several factors make it more likely you will get kidney stones. Some of these you can control, and others you cannot.
Risk factors you can control
Risk factors for both new and recurring kidney stones that you can control include:
- Fluids you drink.
- The most common cause of kidney stones is not drinking enough water. Try to drink enough water to keep your urine clear (about 8 to 10 glasses of water a day).
- Drinking grapefruit juice may increase your risk for developing kidney stones.
- Diet. If you think that your diet may be a problem, schedule an appointment with a dietitian and review your food choices.
- Vitamins C and D can increase your risk of kidney stones when you take more than the daily recommendations. Read supplement labels carefully, and do not take more than the recommended daily doses.
- Levels of calcium affect your risk of kidney stones. Getting your recommended amounts of calcium combined with a low-sodium, low-protein diet may decrease your risk of kidney stones.
- Diets high in protein, sodium, and oxalate-rich foods, such as dark green vegetables, increase your risk for developing kidney stones.
- Weight and weight gain. Weight gain can result in both insulin resistance and increased calcium in the urine, which can result in a greater risk for kidney stones. In one study, weight gain since early adulthood, a high body mass index (BMI), and a large waist size increased a person's risk for kidney stones.4
- Activity level. People who are not very active may have more problems with kidney stones.
- Medicine. Some medicines, such as acetazolamide (Diamox), or indinavir (Crixivan), can cause kidney stones to form.
Risk factors you cannot control
Risk factors for both new and recurring kidney stones that you cannot control include:
Exams and Tests
Your first diagnosis of kidney stones often occurs when you see your doctor or go to an emergency room because you are in great pain. Your doctor or an emergency medicine specialist will ask you questions, examine you (medical history and physical exam), test your urine, and may do some imaging tests (such as an ultrasound, X-ray, or CT scan) before suggesting treatment. After you pass a stone, your doctor may give you another exam to find out whether you are likely to get kidney stones again.
Tests to diagnose kidney stones
Your doctor may do any of the following tests to help diagnose kidney stones, see where they are located, and determine whether they are causing or may cause damage to the urinary tract
- A noncontrast spiral computed tomography (CT) scan is the preferred test for kidney stones. It is a CT scan of the ureters and kidneys, but the scanner moves in a circle as you move through the machine. This test takes half as long as a standard CT scan, provides better images of the kidneys and other organs, and provides different views of the organs.
- An intravenous pyelogram (IVP) is an X-ray test that can show the size, shape, and position of the urinary tract, including the kidneys and ureters. During IVP, a dye called contrast material is injected into a vein (intravenous, IV) in your arm. Then a series of X-ray pictures is taken at timed intervals. The noncontrast spiral CT replaced this test as the preferred test. See an IVP of a kidney stone
- A retrograde pyelogram may be done if the IVP or CT scan does not provide a diagnosis. Rather then being injected through a vein in your arm, the dye is injected through the tubes that carry urine from the kidneys to the bladder (ureters).
- Urinalysis and urine cultures test your urine. A urinalysis measures several different components of urine, including its acidity (pH) and whether it contains blood. A urine culture tests for a urinary tract infection (UTI).
- An abdominal X-ray (KUB) gives a picture of the kidneys, the tubes that connect the kidneys to the bladder (ureters), and the bladder. It may identify a kidney stone. You may also have this test a few weeks after passing the stone to make sure the entire stone passed (if the stone was originally visible by X-ray).
- An ultrasound exam of the kidneys (ultrasonogram) uses reflected sound waves to produce a picture of the kidneys. This is the preferred test for pregnant women.
Tests to determine what type of kidney stone formed
Determining the type of your kidney stone will help with treatment decisions and measures to prevent stones from forming again. Tests to determine the type of stone include:
- A medical history and physical exam focused on determining your risk for more kidney stones. This includes questions about your diet, lifestyle habits, and medical conditions that may make it easier for stones to form.
- Stone analysis. Your doctor may ask you to collect stones by straining your urine through a fine-mesh strainer or fine gauze. He or she will then determine what type of stone it is.
- Blood chemistry screen, to measure kidney function, levels of calcium, uric acid, phosphorus, electrolytes and other substances that may contribute to stone formation. This test can help your doctor determine your chance of having stones in the future.
- Urine collection for 24 hours, to measure volume, pH, calcium, oxalate, uric acid, and other substances that may contribute to stone formation.
You may not have the above tests. Some doctors do them routinely, and others do them only if they feel you may have more stones in the future. Your doctor generally suggests them if you passed more than one stone and if you have a family history of stones.
Women of childbearing age may get a pregnancy test to make sure that pregnancy is not the cause of symptoms and that it is safe to take X-rays
Treatment Overview
Your first diagnosis of kidney stones often occurs when you see your doctor or go to an emergency room because you are in great pain. Your doctor may suggest that you wait for the stone to pass and take pain medicine or have a procedure to remove the stone.
Most small stones [less than 5 mm (0.2 in.)] move out of the body (pass) without the need for any treatment other than taking pain medicine and drinking enough fluids.
- The smaller a stone is, the more likely it is to pass on its own. About 9 out of every 10 stones smaller than 5 mm (0.2 in.) and about 5 out of every 10 stones 5 mm (0.2 in.) to 10 mm (0.4 in.) pass on their own. Only 1 or 2 out of every 10 kidney stones need more than home treatment.
- The average time a stone takes to pass ranges between 1 and 3 weeks, and two-thirds of stones that pass on their own pass within 4 weeks of when the symptoms appeared.
Not all kidney stones are diagnosed because of immediate symptoms. Your stone may not be causing you pain, and your doctor may find it during a routine exam or an exam for another condition or disease. In this case, you have the same treatment options as noted below.
Treatment for your first stone
If your doctor thinks the stone can pass on its own, and you feel you can deal with the pain, he or she may suggest home treatment, including:
- Using pain medicine. Nonprescription medicine, such as nonsteroidal anti-inflammatories (NSAIDs), may relieve your pain. Your doctor can prescribe stronger pain medicine if needed.
- Drinking enough fluids. You'll need to keep drinking water and other fluids when you are passing a kidney stone. If you don't get enough fluids, you could get dehydrated. Drink enough fluids to keep your urine clear, about 8 to 10 glasses a day. If you have kidney, heart, or liver disease and are on fluid restrictions, talk with your doctor before increasing your fluid intake.
Your doctor may prescribe medicine to help your body pass the stone. Alpha-blockers have been shown to help kidney stones pass more quickly with very few side effects. Ask your doctor if these medicines can help you.
If your pain is too severe, if the stones are blocking the urinary tract, or if you also have an infection, your doctor will probably suggest medical or surgical treatment. Your options are:
- Extracorporeal shock wave lithotripsy (ESWL). ESWL uses shock waves that pass easily through the body but are strong enough to break up a kidney stone. This is the most commonly used medical treatment for kidney stones. See a picture of ESWL.
- Ureteroscopy. The surgeon passes a very thin telescope tube (ureteroscope) up the urinary tract to the stone's location, where he or she uses instruments to remove the stone or break it up for easier removal. Occasionally, you may need a small hollow tube (ureteral stent) placed in the ureter for a short time to keep it open and drain urine and any stone pieces. Ureteroscopy is often used for stones that have moved from the kidney to the ureter. See a picture of ureteroscopy.
- Percutaneous nephrolithotomy or nephrolithotripsy. The surgeon puts a narrow telescope into the kidney through a cut in your back. He or she then removes the stone (lithotomy) or breaks it up and removes it (lithotripsy). This procedure may be used if ESWL does not work or if you have a very large stone. See a picture of nephrolithotomy.
- Open surgery. The surgeon makes a cut in the side or the belly to reach the kidneys and remove the stone. This treatment is rarely used.
Preventing future stones
After you have had a kidney stone, you are more likely to have one again. Almost half of all people who have a stone will have more stones within 5 years unless they take preventive measures. You may be able to prevent getting more kidney stones by drinking more fluids and making changes in your diet. If you have risk factors for having more stones, such as a family history of stones, your doctor may suggest medicines that help prevent stones from forming.
What To Think About
Your doctor may ask you to collect your urine for 24 hours after you pass a stone so your urine can be tested to find out the type and cause of the stone. Knowing the type of stone can help determine what you can do to avoid having another.
In rare cases, a person forms kidney stones because the parathyroid glands produce too much of a hormone, which leads to higher calcium levels and possibly calcium kidney stones. To help prevent stones from coming back, your doctor may suggest surgery to remove a parathyroid gland or glands (parathyroidectomy).
You may require more treatment for your kidney stones if you have continuing problems and:
Prevention
If you have more than one kidney stone, especially if you have a family history of stones, you are more likely to have kidney stones again. But you can take steps to help prevent them:
- Drink more fluids. Try to drink enough water to keep your urine clear, about 8 to 10 glasses of water per day. Slowly increase how much you drink, perhaps adding one more glass of water a day until you are drinking 8 to 10 glasses a day. This slow increase will give your body time to adjust to the extra fluids. You are drinking enough water when your urine is clear or light yellow. If it is dark yellow, you are not drinking enough fluids. If you have kidney, heart, or liver disease and have fluid restrictions, talk with your doctor before increasing how much you drink.
- Change your diet. This may be helpful, but it depends on what is causing your kidney stones. Your doctor may do more tests before deciding whether changing your diet will help reduce your risk for developing another stone. The results of these tests may suggest that it could be helpful to do one or more of the following:
- Increase how much fiber you eat. Fiber includes oat bran, beans, whole wheat breads, wheat cereals, cabbage, and carrots.
- Eat less beef, pork, and poultry.
- Eat a moderate or high amount of calcium-rich foods, such as dairy products. Getting your recommended amounts of calcium, combined with a diet low in sodium and protein, may decrease your risk of kidney stones.
- Try not to drink grapefruit juice. Drinking grapefruit juice may increase your risk for developing kidney stones.
- Avoid foods that are high in oxalate, such as dark green vegetables, nuts, and chocolate.
- Try not to add salt when you cook or eat. Try removing the salt shaker from your table.
- Surgery
- People rarely need open surgery to treat kidney stones. In most cases, other less invasive treatments are successful. You may need open surgery when the kidney stone is causing severe bleeding that cannot be controlled. In this case, the surgeon makes a cut in your side or stomach to reach the kidneys, and he or she removes the stone.
- Another type of surgery, percutaneous nephrolithotomy or nephrolithotripsy, is also used. The surgeon puts a narrow telescope into your kidney through small cuts in your back. He or she then removes (lithotomy) or breaks up and removes (lithotripsy) the stone. This surgery may be used if other procedures do not work or if you have a very large stone. See a picture of nephrolithotomy.
- In rare cases, a person forms kidney stones because the parathyroid glands produce too much of a hormone, which leads to higher calcium levels and possibly calcium-type kidney stones. To help prevent stones from coming back, your doctor may suggest surgery to remove a parathyroid gland or glands (parathyroidectomy).
|